Congenital (vertical) Transmission
This topic is one of personal importance, as I believe that I have unknowingly have passed along more than just my witty sense of humor to my son. Like many people I was not aware of my disease before, during or after my pregnancy. It was 13 years later before I even knew my multitudes of autoimmune diagnoses were most likely the result of my immune system being hacked by Borrelia, Babesia , Bartonella, Coxsacki B, and Epstein Barr Virus (EBV). These biofilm quorums had been running amuck disarming my natural defense system.
My difficulties existed prior to my pregnancy which was achieved through In Vitro fertilization (IVF) because of pre-existing hormonal imbalances and adhesions that blocked my fallopian tubes. I had been told my chances of pregnancy were nil naturally and only 30% with each round of IVF treatment. I have never been one to allow odds to determine my path, and despite horrendous hormonal manipulation and invasion procedures I was blessed to get pregnant with twins. During the first trimester I lost one of the babies, no medical explanation was given and I was encouraged to focus on the remaining surviving fetus.
My pregnancy was extremely difficult, nausea, vomiting, gallstones(lost gall bladder 6 weeks post-delivery), weight loss, and pre-partum depression. What was supposed to be the happiest time of my life was fraught with physical, mental and emotional stressors. I would like to say that delivery fared better, but after 3 days of unsuccessful delivery my son joined this world via cesarean section. I did not know at that moment how much I didn’t know.
My health continued to decline resulting in a diagnosis of SLE (systemic Lupus), about 16 months after my son’s birth. At the time there was no concern raised about my son or him acquiring anything but perhaps my temper and looks from me. Over time there have been numerous concerns raised about my sons health and well-being. Suggestions about the possibility of ADHD, or other over stimulation, his coordination and small motor skills developed slower and he continues to have issues with manual dexterity. He has struggled with being overly sensitive to external stimulus, needing more quiet time than most children to slow down and regroup. He continues to struggle with short term memory, numerical dyslexia, sleeping disorder, allergy symptoms , anxiety, and emotional outbursts. Joint pain and tendonitis have been issues since he was 7, he required orthopedic inserts and physiotherapy several times for his knees, ankles and wrists. He has also had motor tic affecting his neck, jaw and shoulders since he was 4/5 years of age.
According to the Pediatric Infectious disease doctor we saw at the Children’s’ Outpatient clinic locally, Lyme is not transmittable from mother to child. That my son has to stop texting late at night to fix his sleeping problems and that he should be assessed for learning problems and ADHD. His sports activities and his growing are what are responsible for his joint issues and he is a teenager, so hormones and normal development can create mental health issues. For certain though, there was NO WAY HE COULD GET LYME FROM ME!
Remington and Klein's Infectious Diseases of the Fetus and Newborn Infant, 8th Edition Copyright 2016
Christopher B. Wilson, MD, Victor Nizet, MD, Yvonne Maldonado, MD, Jack S. Remington, MD and Jerome O. Klein, MD
Update on TORCH Infections in the Newborn Infant
Sue G. Boyer, MN, RN; Kenneth M. Boyer, MD NAINR. 2004;4(1)
The usual way in which the fetus is infected is by transplacental spread after maternal infection in which the organism circulates in the mother's blood. These infections, acquired in utero, can be severe enough to cause fetal loss or can result in intrauterine growth restriction, prematurity, or chronic postnatal infection. In most cases the maternal illness is mild but the impact on the developing fetus is more severe. The degree of severity is dependent on the gestational age of the fetus when infected, the virulence of the organism, the damage to the placenta, and the severity of maternal disease.
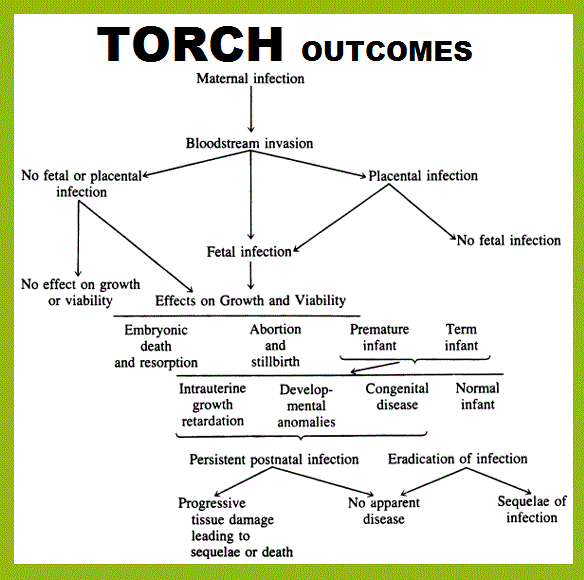
The following research information I will present to you is the result of hours of dedicated in depth research into how wrong this ID doctor was. I have included direct links to each research study so that you can go and learn for yourself. I always recommend people use critical learning skills and to validate all resources and information. I rarely take anyone’s word for anything, I resource my resources, triple check and question the information I find. I suggest you don’t take my word for it, investigate for yourself.
Within the world of Lyme disease research there are many scientists and doctors who have/are trying to uncover the facts behind what we call Lyme disease. I have included excerpts from many well respected professionals who have since the 1980’s known that the Borrelia bacteria as well as other bacteria and viruses are capable of crossing the placental barrier and can be transmitted vertically from mother to fetus. Multiple doctors have acknowledged not only the possibility but have performed research to verify and support their theories. Here is what they specialists in the field have found.

Gestational Lyme borreliosis. Implications for the fetus 1989
Abstract;
Great diversity of clinical expression of signs and symptoms of gestational Lyme borreliosis parallels the diversity of prenatal syphilis. It is documented that transplacental transmission of the spirochete from mother to fetus is possible. Further research is necessary to investigate possible teratogenic effects that might occur if the spirochete reaches the fetus during the period of organogenesis. Autopsy and clinical studies have associated gestational Lyme borreliosis with various medical problems including fetal death, hydrocephalus, cardiovascular anomalies, neonatal respiratory distress, hyperbilirubinemia, intrauterine growth retardation, cortical blindness, sudden infant death syndrome, and maternal toxemia of pregnancy. Whether any or all of these associations are coincidentally or causally related remains to be clarified by further investigation. It is my expectation that the spectrum of gestational Lyme borreliosis will expand into many of the clinical domains of prenatal syphilis.

Infectious Diseases of the Fetus and Newborn Infant, 2001 5th edition, Ed. Remington and Klein. Chapter 11, page 447 – 528.
“Mothers with active Lyme Disease: Treated: 14.6% of the pregnancies with sequelae, Untreated: 66.7% of the pregnancies with sequelae, Unknown as to treatment:
30.3% with sequelae, Specific adverse outcomes included:
cardiac 22.7%, neurologic 15.2%, orthopedic12.1%, ophthalmic 4.5%, genitourinary 10.6%,miscellaneous anomalies 12.1%, 2nd trimester demise 12.1%. Highest rate of adverse outcome (72.7%) in women with infection acquired prior to or during first trimester without treatment.”

Canada Disease weekly report, June 4th,1988
Elly Bollegraaf, Disease surveillance division, Bureau of Communicable Diseases Epidemiology, LCDC, Ottawa,Ontario In conjunction with Dr.H. Artsob, and M Garvie LCDC
Health and Welfare Canada
http://publications.gc.ca/collections/collection_2016/aspc-phac/H12-21-1-14-22.pdf

Clinical Manifestations of Lyme Disease in the United States
DAVID H. TROCK, M.D., JOSEPH E. CRAFT, M.D., AND DANIEL W. RAHN, M.D.
Connecticut Medicine June 1989 Volume 53, No. 6
Pregnancy
Adverse fetal outcomes due to maternal-fetal transmission of Lyme disease have been reported, 30-32 but a uniform pattern of congenital malformations has not been identified. Of equal importance, however, is that the majority of such pregnancies are normal. 31 Adverse outcomes include fetal demise with abnormalities of the heart and great vessels, 30, 31 as well as autopsy reports of septal defects and coarctation of the aorta. If Lyme disease is contracted during the first trimester of pregnancy, coincident with cardiac organogenesis, an increased risk of fetal cardiac anomalies may be present. Other adverse outcomes, which occurred despite antibiotic therapy, have included syndactyly, cortical blindness, and fetal wastage. 31
https://archive.org/stream/connecticutmedic5311conn/connecticutmedic5311conn_djvu.txt

Medical Science Steps Up Its Assault on Lyme Disease
New York Times July 4, 1989
Dr. David Axelrod, the New York State Health Commissioner.
''We do know that the Lyme bacterium crosses the placenta,'' said Dr. David Axelrod, the New York State Health Commissioner. ''Most babies born of mothers with treated Lyme disease have been healthy, yet the long-term impact of this disease on the developing fetus and the newborn is not entirely clear.''

Maternal-fetal transmission of the Lyme Disease spirochete, B. burgdorferi. Ann Intern Med. 1985
Schlesinger PA, Duray PH, Burke BA, Steere AC, Stillman MT.
“Although the number of spirochetes in blood and affected tissues appears to be low, it is clear that the organism may invade and persist in many different sites. The Lyme spirochete may also spread transplacentally to organs of the fetus.” “At the time of childbirth the placenta should be examined for histologic abnormalities and for spirochetes , as in congential syphilis. If the infant is ill, a diagnosis of congenital Lyme disease should be considered.
Mothers with active Lyme Disease,Treated: 14.6% of the pregnancies with sequelae, Untreated: 66.7% of the pregnancies with sequelae, Unknown as to treatment: 30.3% with sequelae. Specific adverse outcomes included:cardiac 22.7%, neurologic 15.2%, orthopedic 12.1%, opthalmic 4.5%,genitourinary 10.6%, miscellaneous anomalies 12.1%, 2nd trimester demise 12.1%. Highest rate of adverse outcome (72.7%)in women with infection acquired prior to or during first trimester. Pregnant woman developed Lyme disease during her first trimester, but did not receive antibiotic therapy. Her infant, born at 35 weeks gestational age, died of congenital heart disease during the first week of life. Histologic examination of autopsy material showed the Lyme disease spirochete in the spleen, kidneys and bone marrow of the infant.
In closing, I have many other studies, articles and research to dig through to add to this current collection. My son and I take each day as it comes, we focus on supporting our immune systems and reducing our exposure to toxins of many kinds. We do not need any label or diagnosis to know what our reality is. One of the last things I said to the Peds ID doctor was that I will enjoy chatting with him again when he learns to admit the truth. I'm ready for the discussion now, I do not believe he or PHAC are however.
Pregnancy and Tick-borne Diseases: Gestational Lyme ILADS CONFERENCE Toronto 2011
graduated from New York Medical College, interned in pediatrics at St. Luke's Medical Center in Manhattan and became chief resident there. He went on to become attending physician at Memorial Sloan-Kettering Cancer Center. Dr. Jones moved to Hamden CT to practice pediatrics in the late 1960s. Within a few months after arriving, he noticed clusters of patients diagnosed with Juvenille Rheumatoid Arthritis, who really had Lyme disease. Since then, Dr. Jones has treated more than 10,000 children for Lyme disease from virtually every state, and from around the world
http://www.youtube.com/watch?v=_O3ySdGMY2g

